When the Bladder Never Feels Truly Calm
For some people, the urge to use the bathroom isn’t just occasional — it’s constant, unpredictable, and often painful.
Interstitial Cystitis (IC), also called painful bladder syndrome, can turn simple routines like travel, sleep, or sitting through a meeting into daily challenges. The discomfort may fluctuate, flare suddenly, or persist despite treatment, creating both physical strain and emotional fatigue.
Standard medical therapies, dietary changes, and pelvic floor care remain the foundation of symptom management. Yet as patients search for additional ways to cope with chronic pelvic pain and bladder sensitivity, one question continues to surface:
Can medical cannabis help reduce Interstitial Cystitis symptoms — or could it introduce new risks?
Let’s examine what current research and clinical experience suggest.
Interstitial Cystitis (IC), also called painful bladder syndrome, can turn simple routines like travel, sleep, or sitting through a meeting into daily challenges. The discomfort may fluctuate, flare suddenly, or persist despite treatment, creating both physical strain and emotional fatigue.
Standard medical therapies, dietary changes, and pelvic floor care remain the foundation of symptom management. Yet as patients search for additional ways to cope with chronic pelvic pain and bladder sensitivity, one question continues to surface:
Can medical cannabis help reduce Interstitial Cystitis symptoms — or could it introduce new risks?
Let’s examine what current research and clinical experience suggest.
Understanding Interstitial Cystitis
Interstitial Cystitis is a chronic condition characterized by bladder pressure, pelvic pain, and urinary urgency without a clear infection.
- Common symptoms include:
- Persistent pelvic or bladder pain
- Frequent urination (sometimes dozens of times daily)
- Urgency even with small urine volumes
- Pain during or after bladder filling
- Disrupted sleep due to nighttime urination
- Discomfort during sexual activity
- IC is considered a complex condition involving multiple biological mechanisms such as:
- Internal Bladder lining (urothelial) dysfunction
- Nerve hypersensitivity
- Chronic inflammation
- Pelvic floor muscle tension
- Central pain processing changes
- Because triggers and severity vary widely, treatment plans must be individualized.
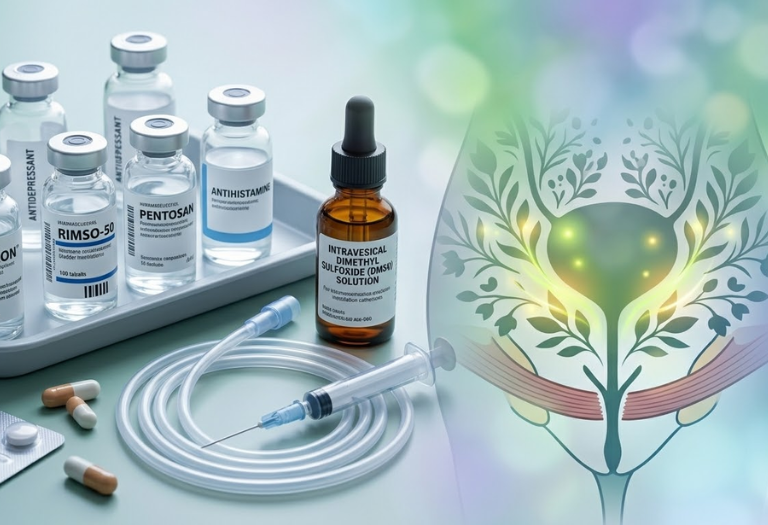
Standard Medical Treatments for Interstitial Cystitis

Medical cannabis is not considered a primary treatment for IC. First-line management typically includes:
1. Bladder and Lifestyle Modifications
Avoiding dietary triggers such as caffeine, alcohol, acidic foods, and artificial sweeteners can help reduce symptom flares.
2. Oral Medications
Options may include antihistamines, tricyclic antidepressants, or bladder-protective agents like pentosan polysulfate sodium.
3. Pelvic Floor Physical Therapy
Many patients benefit from specialized therapy to reduce muscle tension and nerve sensitivity.
3. Pelvic Floor Physical Therapy
Many patients benefit from specialized therapy to reduce muscle tension and nerve sensitivity.
4. Bladder Instillations or Procedures
In more severe cases, doctors may recommend bladder treatments or neuromodulation therapies.
Cannabis, when considered, is typically explored as adjunct symptom support rather than disease-targeted therapy.
The Endocannabinoid System and Bladder Pain
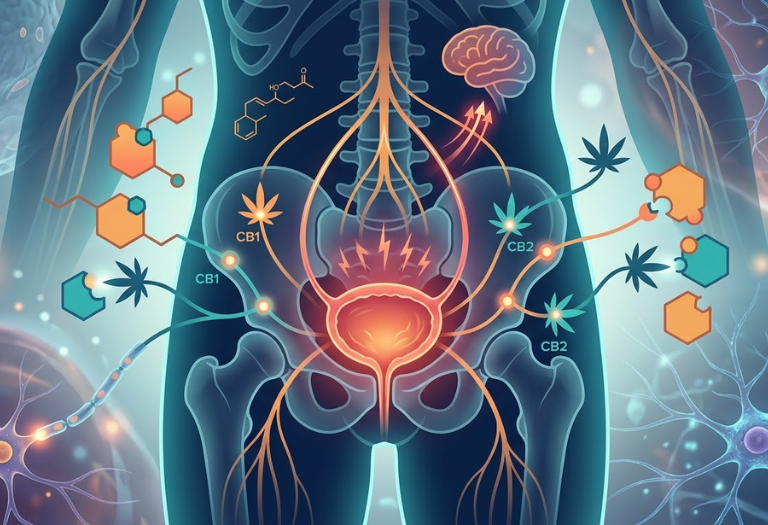
The endocannabinoid system (ECS) helps regulate pain perception, inflammation, stress response, and nerve signaling.
Cannabinoid receptors have been identified in:
- Bladder tissues
- Peripheral nerves
- Spinal cord pain pathways
- Brain regions involved in pain modulation
THC (tetrahydrocannabinol)
- Psychoactive
- May reduce pain perception
- May promote muscle relaxation
- Higher doses may increase anxiety or cognitive impairment
CBD (cannabidiol)
- Non-intoxicating
- May reduce inflammation and anxiety
- May support sleep and emotional regulation
- Often preferred for daytime symptom management
The key question is how these effects translate specifically to IC symptom patterns.
Potential Benefits of Medical Cannabis for IC
Research remains limited, but some patients explore cannabis for symptom relief.
1. Pelvic Pain Reduction
Chronic bladder pain may involve nerve hypersensitivity. THC’s interaction with pain pathways may help some individuals experience reduced discomfort.
2. Urinary Urgency and Muscle Relaxation
Cannabinoids may influence smooth muscle tone and nerve signaling, potentially reducing urgency in certain cases.
3. Sleep Support
Frequent nighttime urination can disrupt restorative sleep. Balanced cannabinoid formulations may help some patients fall asleep more easily.
4. Stress and Anxiety Regulation
Stress can worsen IC flares. CBD’s calming effects may support nervous system stability.
5. Improved Coping with Chronic Symptoms
For some individuals, cannabis may help reduce symptom-related distress and improve quality of life.
Responses vary significantly between patients.

Risks and Considerations
Cannabis use in chronic bladder conditions requires careful evaluation.
1. Symptom Masking
Pain relief may delay recognition of worsening disease or other urological conditions.
2. Cognitive and Psychological Effects
High-THC doses can cause anxiety, dizziness, or impaired concentration.
3. Dependency Potential
Chronic pain patients may be at higher risk of developing cannabis use disorder.
4. Urinary Function Changes
Cannabis may alter bladder signaling in unpredictable ways.
5. Mental Health Contraindications
High-THC products may worsen symptoms in individuals with:
Bipolar disorder
Psychosis spectrum conditions
Severe panic disorder
Professional screening is important before use.
Safer Cannabis Use Strategies for IC Patients

If medical cannabis is recommended within a broader treatment plan:
1. Prioritize CBD-Dominant Products
These may provide symptom support with fewer psychoactive effects.
2. Start Low and Increase Gradually
Microdosing helps monitor how pelvic pain and urgency respond.
3. Choose Controlled Delivery Methods
Tinctures, capsules, or measured edibles provide more predictable dosing than smoking.
4. Track Symptom Changes
Monitor:
- Pain intensity
- Urination frequency
- Sleep quality
- Anxiety levels
Cannabis and IC Medications: Interaction Considerations
Cannabinoids are metabolized through liver enzyme pathways that also process many medications used for IC.
Potential interaction concerns include:
- Antidepressants
- Antihistamines
- Pain medications
- Muscle relaxants

FAQs

1. Can medical cannabis cure Interstitial Cystitis?
No. IC is a chronic condition requiring ongoing symptom management.
2. Can cannabis reduce bladder pain?
Some patients report reduced pelvic pain, but responses vary widely.
3. Is CBD better than THC for IC symptoms?
CBD is generally better tolerated and less likely to cause anxiety or impairment.
4. Can cannabis reduce urinary urgency?
It may help in some cases by affecting nerve signaling, but evidence is limited.
5. Is cannabis approved specifically for IC treatment?
No cannabis-based medications are currently approved specifically for IC.
6. Can cannabis improve sleep disrupted by IC?
Some individuals report better sleep with balanced cannabinoid formulations.
7. Are there risks of dependency?
Yes. Regular high-dose use may increase the risk of cannabis use disorder.
8. Can cannabis interact with IC medications?
Yes. Cannabinoids may affect how certain drugs are metabolized.
9. Should cannabis replace pelvic floor therapy or medications?
No. It should only be considered as complementary support.
10. Should I consult a doctor before trying cannabis for IC?
Yes. Proper evaluation helps ensure safe and appropriate use.
A Balanced Clinical Perspective

Seek prompt evaluation if you experience:
- Blood in urine
- Severe or sudden worsening pelvic pain
- Fever or signs of infection
- Inability to urinate
- Rapid symptom progression

Moving Toward Sustainable Relief
Chronic bladder pain conditions rarely improve with quick fixes. Sustainable relief comes from consistent care, informed choices, and collaboration with healthcare professionals.
If medical cannabis becomes part of your symptom-support strategy, it should be approached thoughtfully — with medical guidance, legal compliance, and careful monitoring.
Because managing chronic pelvic pain isn’t just about relief today — it’s about stability for the long term.
If medical cannabis becomes part of your symptom-support strategy, it should be approached thoughtfully — with medical guidance, legal compliance, and careful monitoring.
Because managing chronic pelvic pain isn’t just about relief today — it’s about stability for the long term.
Ready to find the
perfect strain for your needs?
Navigating the complexities of medical marijuana laws can be tricky, but with the right information, you can protect your privacy and your rights as a medical cannabis cardholder. At Marijuana Specialist Near Me, we make the process of obtaining a medical marijuana card straightforward, with online consultations and guidance through the legal landscape, ensuring you’re well informed about how your card can be used without compromising your privacy.


